Urinary Tract Infection (UTI) Test Strips for Men: Accuracy, Interpretation, and Responsible Use

Urinary tract infections (UTIs) in men are less common than in women, but when they occur, they often require careful evaluation. Unlike uncomplicated bladder infections, UTIs in men are frequently associated with underlying conditions, which makes early assessment especially important.
Many men use an at-home UTI test or a urine dipstick test as a first step when symptoms appear. UTI test strips and UTI test kits offer a convenient way to detect possible infection, but understanding what these tests measure and what they cannot confirm is essential. This guide explains how urinary tract infection test strips work, how accurate an at-home UTI test can be, and when a professional medical evaluation is necessary.
What Is a UTI for Men?
A urinary tract infection (UTI) is a bacterial infection affecting the urinary tract, including the bladder, urethra, kidneys, or prostate gland. In most cases, the causative agent is bacteria that enter the urinary tract, ascending through the urethra. Mild forms of infection may be limited to the bladder, while more severe forms may involve the kidneys or prostate.
Infection in men is frequently associated with anatomical and functional factors. The longer urethra reduces the likelihood of ascending bacterial spread, while prostatic secretions have antibacterial properties. Thus, the occurrence of infection in men more frequently suggests the existence of concomitant risk factors.
For this reason, urinary tract infections in men are often considered potentially complicated. It can be related to obstruction, prostate disease, or other urological disorders that need more thorough diagnosis and clinical assessment.
Common Underlying Causes and Symptoms
The development of urinary tract infections in men is usually associated with impaired urine flow or involvement of the prostate gland. Urinary retention, obstruction, or inflammation of the prostate create conditions for bacterial growth and increase the risk of infection spreading. The most common causes include:
- Prostatitis (inflammation or infection of the prostate gland);
- Benign prostatic hyperplasia (BPH), which impedes urine flow;
- Urinary tract obstruction or urinary stones;
- Recent urological procedures or catheterization.
Clinical manifestations may vary depending on the location of the infection and the age of the patient. The most common symptoms are dysuria, frequent or urgent urination, nocturia, and changes in the appearance or smell of urine. In older men, symptoms may be atypical, with non-specific manifestations such as general weakness, fever, or even confusion without pronounced urological complaints.
What UTI Test Strips Measure
Urine dipstick tests detect chemical markers in urine that may indicate the presence of infection. Unlike laboratory urine analysis (urinalysis), they do not detect bacteria directly, but assess biochemical changes associated with their presence and the body's inflammatory response.
Two indicators are of greatest clinical significance: nitrites and leukocyte esterase. Other parameters may complement the overall picture, but do not confirm infection on their own, and can be seen in the illustration below:
|
Parameter |
What it indicates |
Diagnostic value |
|
Nitrite |
Presence of nitrate-reducing bacteria |
High specificity |
|
Leukocyte esterase |
White blood cells (inflammation) |
Moderate sensitivity |
|
Blood |
Irritation or infection |
Supportive only |
|
Protein |
Inflammation or irritation |
Non-specific |
|
pH |
Urine acidity level |
Context only |
In practical terms, it is nitrites and leukocyte esterase that determine the informative value of the test. Nitrites indicate the metabolic activity of certain bacteria, while leukocyte esterase reflects the body's inflammatory response. The most indicative is the assessment of their combination: the simultaneous presence of both markers significantly increases the likelihood of a bacterial infection, while their absence reduces it, but does not completely rule it out.
Accuracy and Limitations of Dipstick Testing
Dipstick testing is one of the main screening tests that determines the possibility of bacterial infection using indirect markers, including nitrites and leukocyte esterase. It assesses indirect signs of infection, but fails to determine the pathogen or its resistance to antibiotics.
The accuracy of dipstick testing depends largely on the conditions under which the sample is collected. For example, morning urine can be more informative since the longer the bacteria are in contact with urine in the bladder, the higher the chances of identifying nitrites. The reaction may be absent or weak even in the presence of infection when the testing method or interpretation of results is invalid, and may be inaccurate when:
- insufficient time for the urine to remain in the bladder;
- infection with bacteria that do not produce nitrites (e.g., Enterococcus spp.);
- improper technique for collecting the midstream urine sample;
- incorrect timing of reading the result;
- excessive dilution or contamination of the sample.
According to a study by BMJ Journals, “the sensitivity and specificity of urine dipstick tests compared to bacteriological culture were 87% and 45%, respectively, and the negative predictive value was up to 95%,” which highlights their limited role in definitive diagnosis.
Dipstick testing, therefore, allows for a quick assessment of the risk of infection, but its results should not be considered in isolation. Laboratory data, symptoms, and clinical context are the most informed decision-making factors in further management. In order to comprehend the practical importance of these restrictions better, one should take into consideration the correlation between sensitivity and specificity.
Nitrite vs Leukocyte Esterase: Sensitivity and Specificity in Practice
In practice, the difference between sensitivity and specificity becomes important not at the theoretical level, but at the decision-making level. One indicator reduces the risk of missing an infection, while the other reduces the risk of false positives.
|
Indicator |
Nitrite |
Leukocyte esterase |
|
Advantage |
High specificity – a positive result is almost always associated with a bacterial infection |
Low or moderate sensitivity – many infections may be overlooked |
|
Restriction |
Higher sensitivity – better at detecting inflammation |
Lower specificity – false positive results are possible |
In a clinical context, it is the combination of indicators that is important, rather than each one individually.
- Nitrite (+) + LE (+) → high probability of bacterial infection, especially if symptoms are present;
- Nitrite (-) + LE (+) → infection may still be present, and results should be interpreted together with symptoms and risk factors;
- Nitrite (-) + LE (-) → infection is less likely, but further diagnosis is necessary if symptoms persist.
The practical value of the test lies in changing the clinical probability of infection depending on the combination of indicators. It is the assessment of the combination of results that allows for determining the feasibility of further examination or observation.
How to Use UTI Test Strips at Home
The correct technique for using UTI test strips directly affects the accuracy of the result. Even minor violations can alter the reaction of nitrites or leukocyte esterase. The basic steps for correct measurement are listed below:
- It is advisable to use morning urine.
Prolonged contact of bacteria with urine in the bladder increases the likelihood of nitrite detection. - Prepare a clean container for the sample.
Use a sterile or new dry container. Contamination with skin cells, secretions, or detergent residues may cause false positive results. - Collect a midstream urine sample.
Direct the first few seconds of urination into the toilet, then collect the midstream sample in a container. This approach reduces the risk of contamination from bacteria in the urethra or on the skin. - Dip the test strip for 1-2 seconds.
Completely soak the reagent zones, but do not exceed the recommended time. - Remove excess fluid.
Gently shake the strip or run its edge along the container. Do not allow the reagent zones to mix. - Follow the exact measurement time.
Each parameter has its own reaction interval (usually 60–120 seconds). Measuring too early or too late may distort the result. - Compare the color to the scale in good lighting.
Do not interpret the result a few minutes after the reaction is complete, as the color may change.
The diagram below summarizes the sequence of actions when using a test strip:
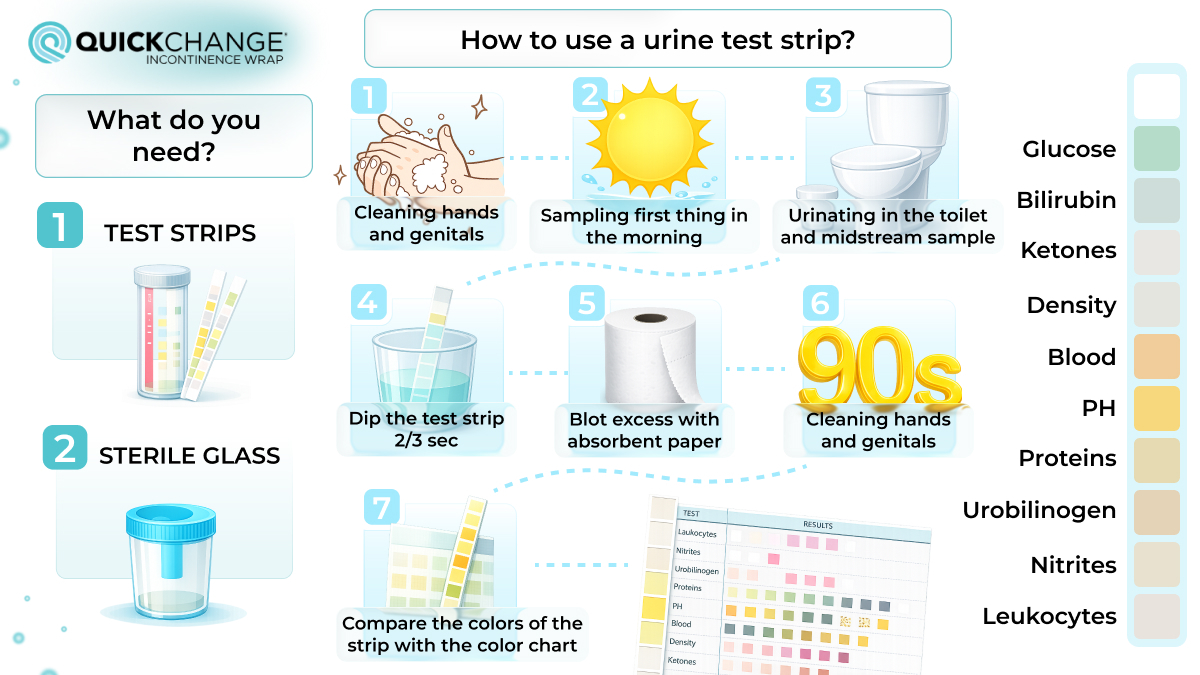
Home Testing vs Medical Evaluation
Dipstick strip home testing may be helpful in the preliminary evaluation of symptoms, but it is not a replacement for clinical examination. Further action should be determined by the severity and duration of symptoms, and the presence of risk factors. A list of circumstances where home testing is suitable and where medical advice is required is as follows:
|
Criterion |
Home testing is appropriate |
Medical consultation is required |
|
Symptom intensity |
Symptoms are mild and not progressing |
Symptoms persist or worsen |
|
Systemic manifestations |
Absent |
Fever, chills, or lower back pain present |
|
Recurrence |
Monitoring for recurrent episodes |
Test results are repeatedly positive |
|
Risk factors |
No known urological conditions |
Prostate disease, obstruction, or recent interventions present |
This can help quickly assess the likelihood of infection, but if you have systemic symptoms or risk factors, you should not delay seeing a doctor. Final confirmation of infection is made through laboratory testing, including bacteriological urine culture.
Digital and Smartphone-Based Test Strip Reading
As at-home UTI test kits become more widely used, digital reading tools have emerged to support interpretation. They use a smartphone camera or dedicated strip readers to analyze color changes in reagent zones, reducing the influence of subjective assessment and lighting errors.
Such systems can improve the reproducibility of results and reduce the risk of misreading, especially when it comes to minor color changes. Special algorithms allow for standardized interpretation and automatic recording of indicators.
At the same time, digital solutions remain auxiliary tools. They do not increase the diagnostic accuracy of the test itself, but only reduce the human factor in reading the results. Therefore, even when using digital systems, the results should be interpreted in a clinical context and, if necessary, confirmed by laboratory tests.
How to Choose UTI Test Strips
The choice of test strips for detecting urinary tract infections should be based not on the number of indicators, but on their diagnostic value and ease of use. Too many parameters do not increase the accuracy of UTI screening and can complicate the interpretation of results without a clinical context.
For adequate home screening, a test strip should contain at least two key indicators, specifically nitrites and leukocyte esterase. The absence of one of them reduces the informative value of the test. Additional parameters do not compensate for their absence.
In addition to these core indicators, it is also important to evaluate several practical product characteristics:
- Balanced strip composition: the test should include both nitrite and leukocyte esterase indicators, which together provide the most informative screening markers for bacterial UTIs;
- Clear instructions on sample collection and reading time: technical errors can lead to false negative or false positive results;
- Contrasting and clear color scale: minimizes subjectivity during interpretation, especially with minor shade changes;
- Current shelf life and proper storage conditions: degradation of reagents reduces the reliability of the test;
- Compliance with regulatory standards, such as FDA clearance for over-the-counter diagnostic devices: indicates quality control and manufacturing standards.
Proper use and storage of test strips directly affect the reliability of results, so the technical characteristics of the product are no less important than the list of indicators.
When to Seek Medical Help
Home testing may be helpful to make a preliminary diagnosis of the symptoms, but there are cases when urgent medical attention is required. Professional assessment can be postponed, which can lead to the further spread of the infection outside the bladder, possibly to the prostate or kidneys.
Immediate medical care is required in case of fever or chills, lower back or side pain, blood in the urine, severe pain during urination, or a positive test strip result repeated. Men with prostate disease, urinary tract obstruction, urinary stones, recent urological procedures or catheterization, or recurrent infections should also consult a doctor.
Recurrent cases of infection demand not only symptomatic therapy but also the discovery of the potential cause. Laboratory urine testing, bacteriological culture, and, in case of need, other urological diagnostics are prescribed in such situations to exclude complications.
Supporting Comfort During Symptom Management
While undergoing diagnosis or awaiting consultation with a doctor, men may need not only clinical evaluation but also practical support in their daily lives. When urological symptoms appear or while waiting for test results, men may experience frequent urination, urgency, or episodes of leakage. During this period, it is important not only to establish a diagnosis, but also to ensure everyday comfort and hygiene.
Products designed for male hygiene can be used as a supportive tool during diagnosis or treatment, complementing rather than replacing medical care. For example, male incontinence support solutions, such as QuickChange Wraps, can be used as a temporary solution to ensure comfort and hygiene while assessment or treatment is ongoing.
Practical continence options, including trial packs for home use and professional sample packs, are available to help address different needs and care settings.
Using Test Strips Responsibly
The use of test strips in men requires special attention, as urinary tract infections in men are more likely to be complicated or associated with concomitant urological conditions. A positive result does not determine the location of the infection (bladder, prostate, or kidneys) and does not allow for an assessment of the severity of the process.
Proper use also involves interpreting the results in the context of symptoms and individual risk factors. A negative dipstick result does not fully exclude infection, and a positive result does not determine the location or severity of the condition.
Particular caution is required in situations where symptoms persist despite a negative test result or when repeated positive results are observed. Self-medication with antibiotics without laboratory confirmation can mask the underlying pathology and contribute to the development of antibiotic resistance. A rational approach is to use the test as a primary assessment tool, followed by professional medical consultation if risk factors are present or symptoms progress.
Conclusion
Urinary tract infection test strips offer a practical way to assess the likelihood of infection when symptoms first appear. Their results are most meaningful when interpreted alongside symptom severity, duration, and individual risk factors, helping guide appropriate next steps.
In men, where UTIs may be linked to underlying urological conditions, careful interpretation and timely medical evaluation are essential. During diagnostic assessment or treatment, maintaining hygiene and managing temporary leakage can help support cleanliness, comfort, and confidence in everyday life. Supportive solutions such as QuickChange Wraps can reduce discomfort and maintain cleanliness, complementing professional medical care.
FAQ
How long does a UTI test take?
A urine dipstick test usually gives results in 1-2 minutes, depending on the parameter under investigation, whereas laboratory urinalysis can take several hours, and a urine culture to verify bacterial growth can take 24-48 hours.
How do doctors test for UTI?
Physicians typically start with urinalysis or a urine dipstick test to identify indicators of leukocytes and nitrites, and in case of suspected infection, they can request a urine culture to identify the bacteria and determine sensitivity to antibiotics, and further testing in men when complications are suspected.
Are at-home UTI tests accurate?
A home UTI test may be used to approximate the risk of infection, particularly when nitrites and leukocyte esterase are both positive, but the results are not as reliable as laboratory confirmation when the symptoms are persistent.
How to read UTI test strips?
UTI test strips are to be read by matching each reactive pad with the colour chart within the given time frame, with adequate lighting, and nitrite and leukocyte esterase results to be read together to make a more accurate evaluation.
This content is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your GP or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay seeking it because of something you have read or seen here.